 It appears that cross-reactivity between penicillins and cephalosporins is more likely associated with structurally similar side chains rather than the beta-lactam ring itself. 5-9 In 1 prospective study, the rate of cross-reactivity among subjects with a positive penicillin skin test was 6%. 4 However, more recent observational studies have found cross-reactivity rates of between 0.17% and 0.7%. This rate derived from early cross-reactivity studies seems to have been caused, at least partially, by contamination of early preparations of cephalosporins with trace amounts of penicillin G. A common myth is that about 10% of patients with a penicillin allergy history will experience an allergic reaction if administered a cephalosporin. 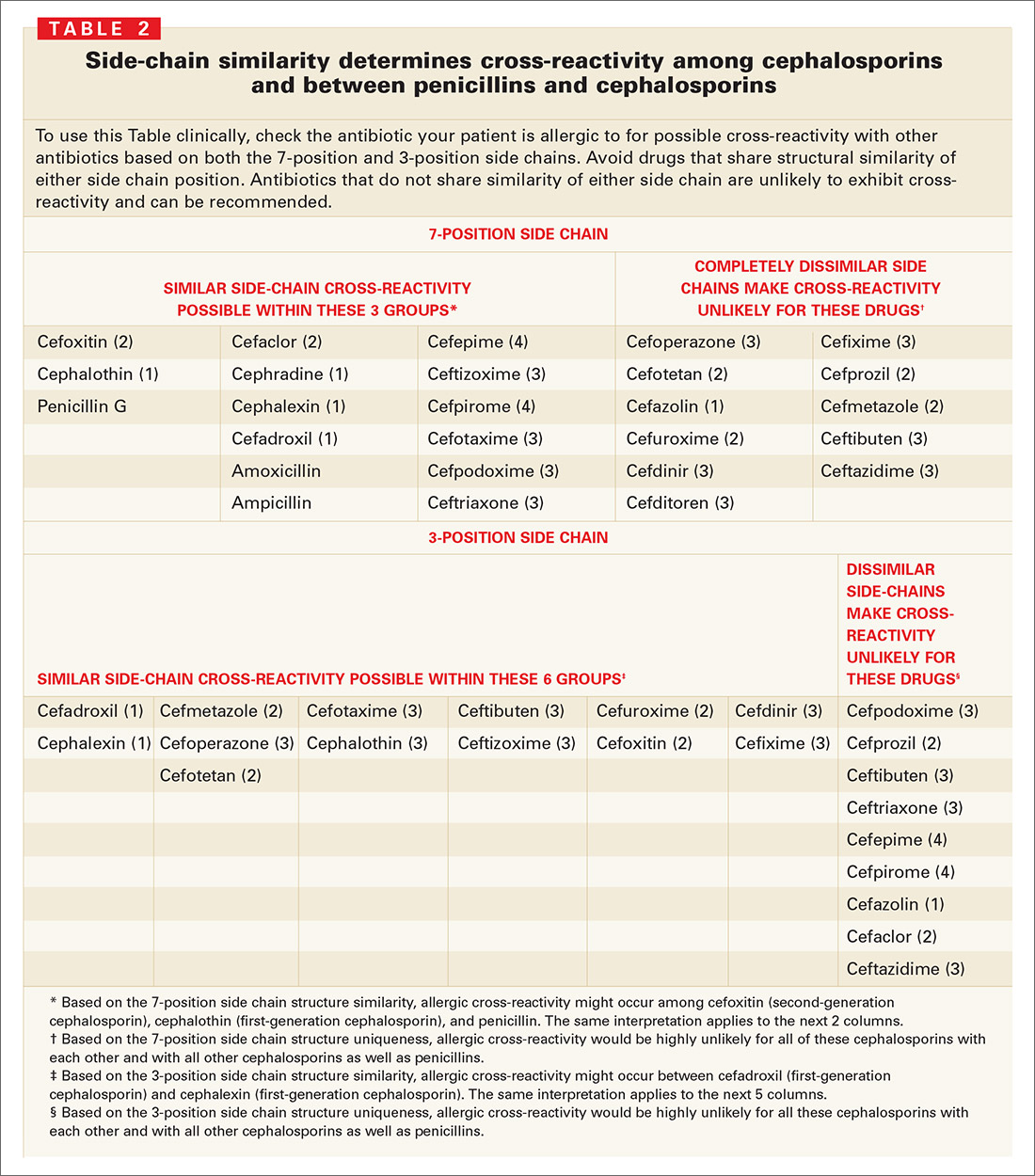
Understanding the possible cross-reactivity will help a provider assess the risk to the patient and ultimately decide whether a nonpenicillin beta-lactam should be used.įor cephalosporins, the rate of cross-reactivity with penicillins is lower than previously believed.  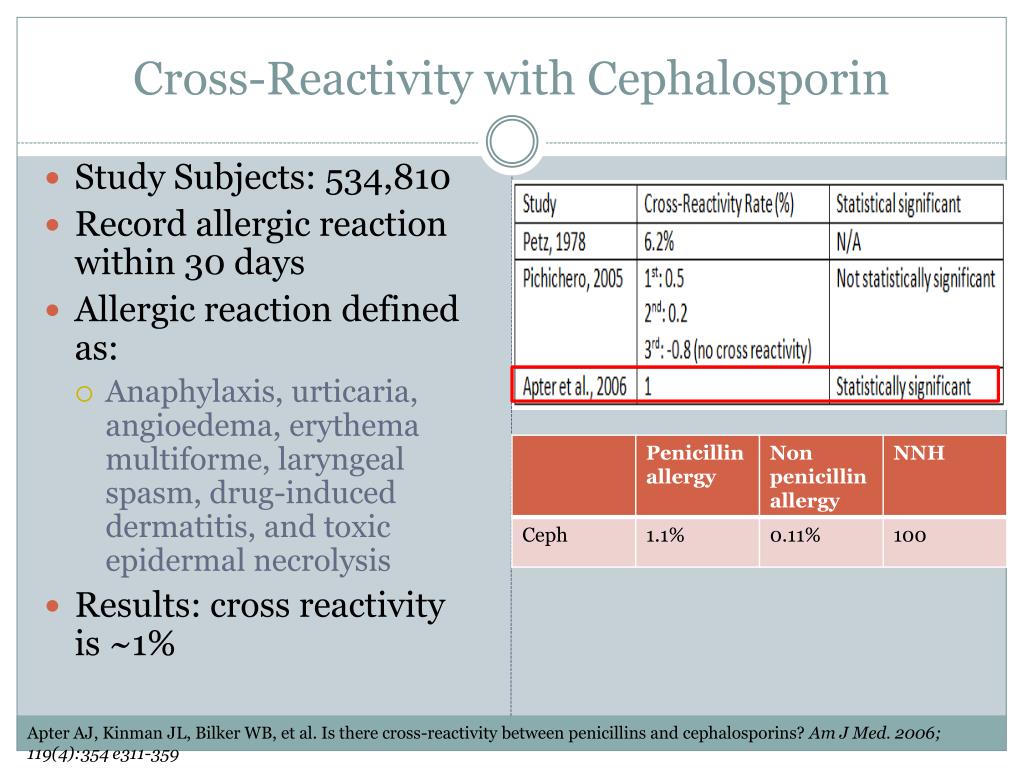
3 If a patient’s penicillin allergy is determined by reaction severity or allergy testing to represent a true allergy, then the clinician is faced with the challenge of determining and interpreting the rate of allergic cross-reactivity from the penicillin class to the other beta-lactam classes (ie, cephalosporins, carbapenems, and mono-bactams). It is important to ascertain a patient’s reported reaction and reaction timing with regard to administration to help indicate whether the allergy represents an immunoglobin (IgE)-mediated reaction, a delayed-onset reaction, an adverse effect, or simply an intolerance. 1 This strategy will frequently lead to suboptimal regimens, including therapies that may be inferior to beta-lactam-based regimens or those that may have unnecessarily broad or inappropriately narrow spectrums of activity. Often, when patients are labeled as having a penicillin allergy, providers are forced to approach the scenario conservatively and simply avoid using beta-lactams. 2 Thus, with a true rate of penicillin allergy likely much lower than that reported by patients, health care professionals are often placed in a predicament regarding the selection of empiric antimicrobial therapy to treat a wide array of infectious conditions. 1 Primary reactions to penicillin antibiotics include rash, itching, nausea and vomiting, shortness of breath, and anaphylaxis.ĭespite the high population prevalence, 80% to 90% of those reporting a penicillin allergy will have a negative response to penicillin skin testing. Thus, our data indicate that cephalosporins can be considered for patients with penicillin allergy.Patient-reported allergy to penicillin antibiotics is a common scenario during health care encounters, with an estimated population prevalence of roughly 8% to 12%. Cross-reactivity is not an adequate explanation for this increased risk, and the risk of anaphylaxis is very low. Patients with allergic-like events after penicillin had a markedly increased risk of events after either subsequent cephalosporins or sulfonamide antibiotics. The unadjusted risk ratio for sulfonamide antibiotic, rather than cephalosporin after penicillin allergic-like events was 7.2 (confidence interval 3.8-13.5). The absolute risk of anaphylaxis after a cephalosporin was less than 0.001%. Among patients receiving a penicillin followed by a cephalosporin, the unadjusted risk ratio of an allergic-like event for those who had a prior event, compared with those who had no such prior event, narrowly defined, was 10.1 (confidence interval 7.4-13.8). Comparison was made with a population of patients receiving a prescription for a penicillin followed by a prescription for a sulfonamide antibiotic.Ī total of 3,375,162 patients received a penicillin 506,679 (15%) received a subsequent cephalosporin. Allergic events were defined by 2 sets of codes: 1 more restrictive, 1 more inclusive. We selected all patients receiving a prescription for penicillin followed by a prescription for a cephalosporin and identified allergic-like events within 30 days after each prescription. We conducted a retrospective cohort study using the United Kingdom General Practice Research Database. We sought to determine the risk of an allergic reaction to a cephalosporin exposure in those with prior penicillin reactions. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
